According to the World Health Organization, depression is the leading cause of disability worldwide. Approximately 300 million suffer from depression, with more women affected than men. A Mayo Clinic study found that 70% of Americans are prescribed medications and anti-depressants are the second-highest prescriptions given. Approximately 1/3 of these people do not get the help they need from anti-depressant drugs. What about turmeric? Does turmeric work for depression?
Anxiety and depression are complex disorders because there are numerous factors including social, environmental, psychological and physical manifestations.
- Our interpersonal relationships and career can lead to chronic stress and the suppression of our feel-good neurotransmitters.
- Imbalanced estrogen and progesterone levels in women and low testosterone in men can lead to depression.
- The environment can be a source of toxicity depending on the air, water, and your home, leading to inflammation-induced depression. The climate can affect your mood, with some people feeling worse in heat and others in colder climates with less sun.
- Your digestive health plays a major role in your psychological health due to the gut/brain axis, affecting both nutrient absorption and toxicity levels. Probiotics in your gut are vitamin factories and balance all your neurotransmitters. There also be a connection to your gut bacteria and turmeric for depression.
- A lack of exercise and the extreme end of exercise affect numerous genes that can lead to depression.
The Estrogen and Serotonin Connection to Depression
Prescribed antidepressants target the monoamine (MAO) systems, which are in the estrogen pathway, targeting the neurotransmitters dopamine, serotonin or norepinephrine. While the complexity makes it difficult to pin down the full scope of higher rates of depression, I do want to highlight the serotonin and estrogen pathway because the MAO pathway may help explain how turmeric helps for depression.
In the estrogen pathway, MAO, COMT, and CYP1B1 all govern the speed at which serotonin, estrogen, dopamine, and epinephrine are increased and decreased. Low and high levels of any of these neurotransmitters will lead to depression or anxiety.
Turmeric has been found to be a natural MAO inhibitor, increasing the amount of circulating serotonin, dopamine, and norepinephrine. This is an important point to note if you are already taking an MAO inhibitor because you want to be careful not to cause serotonin syndrome (high levels of serotonin that causes extreme panic and anxiety).
For females, the menstrual cycle gives rise and fall in estrogen, progesterone, and serotonin. As estrogen rises, so does serotonin. As it goes down, so does serotonin. Estrogen influences pain transmission, headache, dizziness, nausea, and depression through serotonin signaling.
When these swings happen in extremes, the feelings of anxiety and depression can be amplified. While serotonin is mainly thought of as a mood-elevating neurotransmitter of the brain, only 1% of serotonin is found in the central nervous system. The remaining 99% is found in the gut and immune tissues regulating gut motility, vasodilation, clotting, immune cells and uterine contractions.
The cravings for sugar and carbohydrates right before your period is your digestive brain’s attempt to bring serotonin levels back up. Add poor gut flora to the equation, and estrogen can become deconjugated, reabsorbed and reactivated in the blood leading to estrogen dominance and wide swings in serotonin.
IBS is a condition of serotonin (and glutamate) rushes and shortages and the consequential estrogen dysregulation.
Fibromyalgia is another condition believed to be linked to estrogen and serotonin levels due to altered tryptophan metabolism (precursor to serotonin) and is observed in more females than males.
Dysregulated Hormones Monthly Cycle
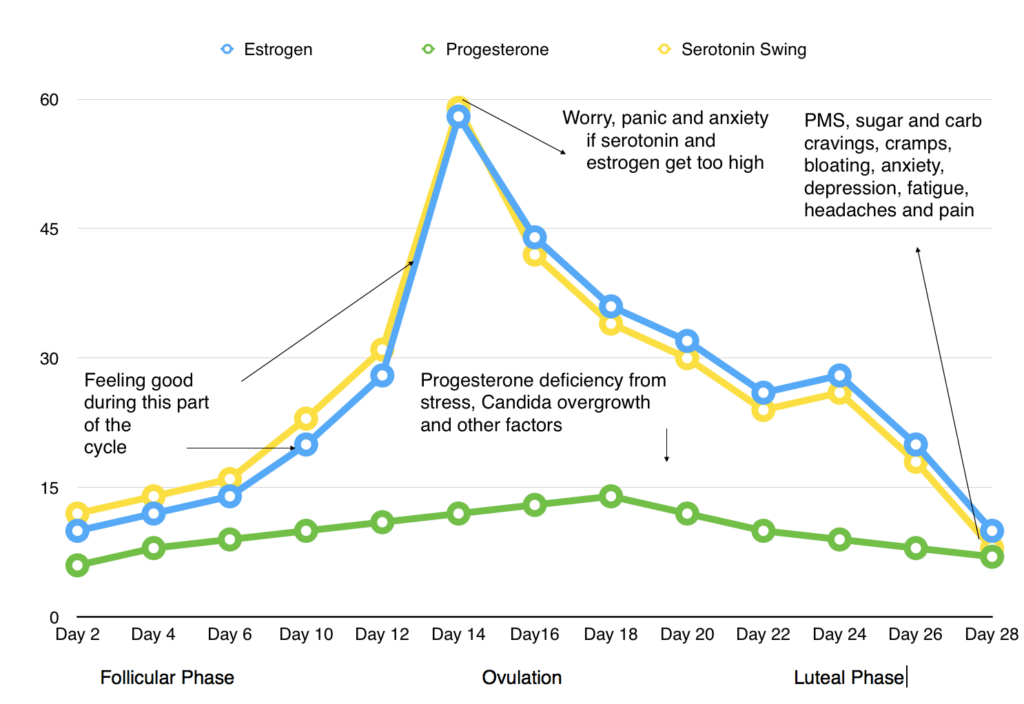
What about post-menopausal women you may be asking? The loss of estrogen at menopause results in a lower activity of serotonin, likely connected to hot flashes and night sweats. Increasing foods high in phytoestrogens like flax seeds during this time period helps bring relief due to phytoestrogens binding to estrogen receptors and upregulating serotonin receptors. Maintaining a diet high in phytoestrogens may assist throughout the post-menopausal period for estrogen and serotonin levels.
The Inflammation Connection and Why Turmeric May Work for Depression
Turmeric has many health benefits, including being a natural anti-inflammatory. Inflammation is another reason why we may look towards the benefits of turmeric for depression. Have you noticed that your cold and flu symptoms also bring depression? We may think that this is an obvious symptom of feeling sick, but what if your immune system is actually dictating how you feel? If you have a chronic illness or low-level inflammation, those inflammatory compounds are going to depress your digestive system (80% of your immune system is in your gut) and the neurotransmitters in your brain (gut/brain axis).
Research has shown that “patients with increased inflammatory cytokines due to a variety of medical illnesses have increased rates of depression compared to the general population.” Therefore, we can consider inflammatory depression as another subtype.
Research has also shown that mania, and to a less extent, depression, occurs in a pro-inflammatory state and that the immune system should be a target for treatment. In this study, the pro-inflammatory cytokines, IL-2, IL-4 and IL-6, were increased in mania subjects in comparison with healthy subjects. Patients in the depressive episodes showed only increased IL-6 levels. Mood symptoms showed a positive correlation with IL-6 and IL-2. Other studies have also found elevated levels of TNF-alpha and C-Reactive Protein.
Chronic exposure to elevated inflammatory cytokines alters the neurotransmitters, which can lead to neuropsychiatric disorders and depression. This includes the serotonin, dopamine, epinephrine, glutamate, and decreases in the brain-derived neurotrophic factor (BDNF), and genetic susceptibilities to low and high levels can be tested in The Nutrition Genome Report. What is causing chronic inflammation? It can be your diet, digestive inflammation, physical or emotional trauma, obesity, chronic stress, poor sleep and genetic polymorphisms.
Mice studies on the gut microbiota have found that manipulation of probiotics altered behavior and BDNF levels independent of changes in inflammatory cytokines. It is almost as if your gut flora circumvents external inflammation, overrides the negative neural signals and improves mood despite elevated cytokines. This may help explain why obesity influences depression due to altered gut flora and high adipose tissue that leads to elevated cytokines.
The anti-inflammatory activity of turmeric is something that should be considered for inflammation-induced depression.
Past Trauma and Depression
When the system has been under extreme duress, there appears to be a hyper response to stressors. Individuals with early life stress have responded to stressors with higher levels of the cytokine IL-6, NF-kB and a decreased ability to inhibit inflammatory cytokines compared to non-depressed controls. This may be rooted in evolutionary survival in that a heightened cytokine response confers greater protection against bacteria and viruses, however, when chronically stimulated, it leads to depression. This can increase the need for a strong-anti-inflammatory to offset oxidative stress.
Interesting enough, research has found that patients who did not respond to antidepressant treatment had higher concentrations of circulating cytokines than patients who respond to antidepressant treatment, extenuating the role of turmeric for depression by lowering inflammation.
How Does Turmeric Work for Depression?
There are many products that claim to be a supplement for depression based on their influence on certain neurotransmitters. It has been my experience that people with chronically low serotonin levels respond best to turmeric. This is the same 33.3 percent group that respond positively to SSRI’s.
Research indicates that turmeric and curcumin treatment may provide benefit by acting on gut microbiota. Currently, there is limited evidence to support this hypothesis, but since 90% of serotonin is made in the gut, there is likely an interaction here along with the MAO serotonin pathway.
How do you know if low serotonin levels are the primary cause of your depression and not issues with dopamine, epinephrine, glutamate, and GABA? It isn’t always just one neurotransmitter, and some people take SSRI’s and a medication like Lamictal to target both serotonin and glutamate.
The hint that turmeric will work depression is poor gut health (chronic use of antibiotics, candida overgrowth, periods of constipation and diarrhea), sugar and flour-based carbohydrate cravings, low motivation to exercise, and simply a lack of motivation to do much at all.
Turmeric root has a full spectrum of mechanisms at work for depression, unlike drugs that trick the body and lead to nutrient depletion and tolerance.
- Moderates hypothalamus–pituitary–adrenal disturbances
- Lowers inflammation
- Protects against oxidative stress from free radicals and mitochondrial damage
- Protects against neuroprogression and intestinal hyperpermeability
Is Turmeric One of the Alternatives to Prozac?
A study from 2014 took 60 patients diagnosed with major depressive disorder and was randomized in a 1:1:1 ratio for six weeks given fluoxetine (20 mg) and curcumin (1000 mg) individually or their combination. The proportion of the responders was highest in the combination group (77.8%) while the Prozac group showed 64.7%and the curcumin group 62.5%.
The researchers, however, concluded that the data was not statistically significant, there was a higher risk of the placebo effect due to the subjects not being blinded, and they were also allowed to take benzodiazepines.
This study should serve to influence further research using a double-blind placebo model. Based on the research to this point, there is evidence that turmeric may be one of the alternatives to Prozac without the side effects.
Should You Use Turmeric or A Curcumin Extract for Depression?
What’s the difference between turmeric and curcumin? Turmeric is a member of the ginger family (Zingiberaceae) and is prescribed abundantly for ailments in both traditional Chinese and Indian medicine. Turmeric extract is isolated curcumin, the active compound (up to 5%) of the spice turmeric. This is the compound you see in the majority of research studies and curcumin supplements.
Major phytoconstituents of turmeric are diarylheptanoids, which occur in a mixture.
- Curcuminoids generally makeup approximately 16% of turmeric.
- Demethoxycurcumin (3, 20, 27%),
- Bisdemethoxycurcumin (4, 10,15%)
- Numerous and less abundant secondary metabolites
A fascinating mechanism known as neurohormesis is when low doses of a substance activate adaptive cellular stress-response pathways in cells and neurons. Phytochemicals such as resveratrol, sulforaphanes, and curcumin might protect neurons against injury and disease through a neurohormetic response to a low dosage that stimulates the production of antioxidant enzymes, neurotrophic factors, and more.
I suspect alcohol in the right dosage also has this effect. Scientists reported in the Chemical Research in Toxicology that phytochemicals in high supplement doses could actually be detrimental to health, especially when combined with certain medications or genetic polymorphisms.
The implications of this understanding his huge. This means that instead of isolating resveratrol, sulforaphane, and curcumin and taking large isolated doses, it is likely that small amounts like those found in wine (resveratrol), broccoli (sulforaphane) and the spice turmeric (curcumin) are more advantageous. Overloading the body with isolated extracts may suppress neurohormesis. Therefore, a low dose of curcumin working in a proportion of the whole root makes more sense than high amounts of isolated curcumin.
What do the Studies Say About Turmeric for Depression?
A 2017 meta-analysis of 6 clinical trials with a total of 377 patients comparing the active ingredient curcumin to a placebo found significant clinical efficacy of curcumin in ameliorating depressive symptoms and anxiety in 3 of the trials. There were also zero reports of adverse events in any of the trials.
What about Turmeric Supplements? How Much Turmeric Should You Take Per Day for Depression?
How much turmeric for depression is the key question? Researchers have found that high doses of curcumin do not necessarily equal more benefits. In fact, low doses of curcumin are believed to be preferable. An oral dose of up to 12 g/day has been given with no adverse effects, but the absorption of the compound has been found to be negligible.
A dosage between 500-1000mg of a full spectrum product is likely how much turmeric to use for depression. Since turmeric has a notoriously poor absorption profile, a fat carrier, and black pepper is necessary to increase absorption.
How Long Does It Take for Turmeric to Work?
If you are not noticing any effect from turmeric, make sure you are using a quality full-spectrum formulation with a fat carrier and black pepper. There are a lot of cheap, poorly made isolated curcumin products on the market. You should notice a difference within 1-2 weeks if turmeric is the right fit for you.
The Health Beat’s Recommend Turmeric Supplements
Along with using turmeric powder in your cooking, the following turmeric supplements are recommended. Talk to your doctor before starting turmeric.
1. PaleoValley Turmeric Complex (15% off with this link)
This product provides 1,000mg of full spectrum turmeric, is tested extensively for purity, and contains coconut oil powder and black pepper to enhance absorption and bioavailability. This formula also includes rosemary, ginger, and cloves, which gives this it an edge for targeting the inflammation root cause of depression.
2. Synergy SuperPure Turmeric Extract
Synergy uses a triple spectrum extract of the whole plant with an essential oil carrier. This superior formula also contains turmerosacchrides that have been found to lower osteoarthritic pain.
2. Gaia Herbs Turmeric Supreme
Gaia’s formula uses a whole plant profile of turmeric with non-GMO lecithin oil carrier and black pepper.







Thank you for the article. I was looking for a comparison of quality between Plexus vitamins and probiotics, which a friend uses and swears by, in comparison to Melaleuca products, which I use. Your articles came up in the search and even though I did not find the answer to my question, I found the information on your website amazing and informative. I have been usuing Mark Frank Tumeric curcurim with peper extract since I had a knee surgery. it reduced inflammation significantly. Other ones I tried did not give me the same results. I take two caps daily which is 1300 mg. What do you think about this product?
Highest Potency Turmeric Curcumin Complex 1400 with BioPerine and Curcuminoids for Absorption, Joint Relief,Anti-inflammatory, Antioxidant, 60 Veggie
Sold by: Marty Frank Naturals
Hi Lynda,
Thank you for the feedback. The product you are using looks fine. I have seen the same results with Meriva SR by Thorne Research for joint pain.
Hello I am a 37 year old female who is dx with anxiety/depression and diabetes and I have 3 children who are vitamin D deficient and also two with ADHD and one with anxiety. There is a lot of good information on your site and I want to try to help myself and kids with a more natural approach, I just don’t know where to start as far as taking multivitamins/supplements, turmeric, vit d drops, omega 3 fish oil. How much to take, how much is too much or not enough, can I do a multivitamin and vit d drops? I would really like you help. Thank you
Hello I am a 37 year old female with 3 kids who all have a deficiency in vitamin d, two with ADHD and one with anxiety. I have also been dx with depression/anxiety and diabetes. I found your website very informal but I don’t know how to go about taking multivitamin/supplements, turmeric, vit d drops, and omega 3 fish oils, how much is too much or not enough, can I use a multivitamin and vit d drops, what is best for kids 6, 8, and 16. I want to help myself and family with a more natural approach but don’t know where to start. I hope you can send me in the right direction, thank you.
Hi Charlene,
I know it can be overwhelming to start. The first step is to start with food for yourself and your children. This will give you a good base for getting your blood sugar under control and promote a healthy gut, which will help ADHD, depression and anxiety. I have set of 10 guidelines for a basic healthy diet, which is a good place to start: https://thehealthbeat.com/about/what-is-paleoedge/
The next step would be a multivitamin from this list: https://thehealthbeat.com/best-worst-multi-vitamins-athletes/
Here are recommendations for children: https://thehealthbeat.com/worst-childrens-multivitamins/
As far as vitamin D, fish oil and turmeric go, this is where having a health practitioner is helpful so that they can give you targeted recommendations and dosages based on your individual needs and health history so that you get results. I have a growing list of recommendations here: https://nutritiongenome.com/consultations/
Thank you so much I really needed to be pointed in the right direction.
Hello, i am using nac in the morning and evening for anxiety, psychosis and depression and drug cravings. It seems to work for me. I just started with C3 sabinsa curcumin for depression because in the past i took long time ssri for depression and anxiety.Is nac and curcumin a safe combination to take long term? Should i take them together or apart and at what time best? I am sorry for my poor english. Best regards. Waldemar
Hi Waldemar,
Your English looks good to me! If NAC is working, that shows you that there is an inflammatory component for you regarding mood. This means that curcumin would likely be an excellent addition. I’m not aware of any interactions or long-term issues with taking NAC and curcumin together. I would check with your doctor, but I don’t believe there is any negative interaction if taken at the same time. Morning and evening supplementation is typically the best approach.
Curcumin has to be the most confusing supplement ever , so many formulations.
https://pureprescriptions.com/scientific-study-reveals-the-best-curcumin-product/
Life extension has released a new product that combines with fenugreek – Elite brand
SmarterNutrition has a new one that uses black cumin seed oil.
Sports Research has one on Amazon you would probably like, uses pepper + coconut oil.
Hi James,
I find myself at odds with curcumin supplementation as well. There’s part of me that thinks curcumin and resveratrol are more advantageous in small amounts due to a hormetic response vs. a larger dose causing an adverse effect. The fact that these compounds are small in foods or drinks and are so poorly absorbed tells me that there is a reason for that. There have been isolated events of elevated liver enzymes with turmeric supplementation, though it is considered rare. There are also positive trials with higher dose curcumin for depression and inflammation and a low rate of adverse effects. So I still don’t think we have a clear understanding of curcumin application, dosing, and formulation.
I have lupus. I am also from the Caribbean where we cook a lot with curry. I have been adding turmeric and black pepper to every dish I cook even my omelettes spinach dish which is so yummy. Inflammation is at 0 for me as is depression. I am 64 and feel like 34. I have to remember how old I am at times because I don’t feel like it. It’s all due to diet. And curry and turmeric/black pepper and spices have a lot to do with it. Thank God got heritage.
Hi Rosemarie,
Thank you for sharing your experience with turmeric! That is so inspiring to hear, and I’m sure it will help others to hear as well.
Turmeric is a spice that has been used for centuries in traditional medicine. It is known for its anti-inflammatory and antioxidant properties.
There is some evidence that turmeric may be helpful for depression. A 2017 review of studies found that turmeric extracts effectively reduced symptoms of depression, anxiety, and stress.
However, more research is needed to confirm the effectiveness of turmeric for depression. It is important to note that turmeric is not a substitute for traditional treatment for depression. If you are experiencing symptoms of depression, it is essential to talk to your doctor.