The Function of Chemotherapy
Chemotherapy may be given as an injection, drip or pill, and exerts its effects on cancer by inducing oxidative stress -mainly superoxide and hydrogen peroxide – to all cells, both normal and cancerous.
Due to the toxic action of chemotherapy, the heart, kidneys, bone marrow, liver and digestive system are highly susceptible to injury. This makes the synergistic support with diet and the best supplementation for chemotherapy a crucial part of a cancer treatment program. Immunotherapy is becoming a superior option to chemotherapy because it uses substances either made by the body or in a lab to improve or restore immune system function. This is exactly what diet and supplementation can also do.
Antioxidants and Chemotherapy: Is there Evidence to Avoid Antioxidants?
A primary mechanism of many chemotherapy drugs against cancer cells is the formation of pro-oxidants or free radicals. The standard protocol for chemotherapy is to discontinue the use of antioxidants with the logic that it may interfere with the pro-oxidant effect of chemotherapy. Chemotherapy generates high amounts of oxidative stress, and therefore it would appear that antioxidants could attenuate the effectiveness of the oxidative stress to kill cancer cells. This, however, is just a theory and has not sufficiently been proven.
Whether to avoid antioxidants or use them during chemotherapy is still considered controversial. The problem is that to avoid all antioxidants during chemotherapy would mean to avoid all meat, fish, whey, fruits, vegetables, nuts, seeds, and herbs. Antioxidants are ubiquitous through endogenous production in our body and in our entire whole food supply. It is also to misunderstand the pro-oxidative effect that some of these compounds have on cancerous cells through oxidative stress without harming healthy cells.
Recommendation Basis to Avoid Antioxidants during Chemotherapy?
If you go through the literature, there is a lot of conflicting opinions regarding the use of antioxidants during chemotherapy. I have not been able to find any definitive evidence for avoiding them.
A 2005 study boldly titled “Use of Antioxidants During Chemotherapy Should Be Avoided” was not based on any conclusive findings. It was based on the fact that “preclinical data is currently inconclusive and a limited number of clinical studies have not found any benefit” regarding antioxidant supplementation.
A study from 2000 found that “several studies suggest that dietary supplementation with antioxidants can influence the response to chemotherapy as well as the development of adverse side effects that results from treatment. It is the increase in oxidative stress that causes gastrointestinal toxicity and mutagenesis. Antioxidants detoxify ROS (oxidative stress) and may enhance the anticancer effects of chemotherapy.”
A study from 2007 did a systematic review of the evidence from 845 articles and 19 randomized controlled trials. They concluded that “none of the trials reported evidence of significant decreases in efficacy from antioxidant supplementation during chemotherapy. Many of the studies indicated that antioxidant supplementation resulted in either increased survival times, increased tumor responses, or both, as well as fewer toxicities than controls.” The need for larger well-designed studies was noted, but there is no evidence showing that antioxidants are negatively affecting treatment.
A study from 2008 found that pre-treatment with vitamin C in mice given doxorubicin, cisplatin, vincristine, methotrexate and imatinib and was found to reduce the effectiveness of the drugs. The mechanism, however, had nothing to do with its antioxidant activity, and instead was hypothesized to possibly be due to vitamin C protecting a cancer cell’s mitochondria. However, later in this article, you will see why I see agree with this theory and that there must have been something different that occurred due to using a cell culture and the timing of the dose.
A study from 2013 stated that “There is still limited evidence in both quality and sample size, suggesting that certain antioxidant supplements may reduce adverse reactions and toxicities. Significant reductions in toxicity may alleviate dose-limiting toxicities so that more patients are able to complete prescribed chemotherapy regimens and thus, in turn, improve the potential for success in terms of tumor response and survival.”
Examples of the Best Supplements During Chemotherapy: The Research
In the following diagram, you can see the process by which chemotherapy generates superoxide and hydrogen peroxide to kill cancer cells. This process happens to healthy cells too. Here is the oxidative stress process, and how antioxidants can support healthy cell protection without disrupting therapy:
Vitamin C
The endogenous enzymatic antioxidant defenses of the body include superoxide dismutase, glutathione peroxidase, and catalase, with nitric oxide playing a major role in balancing oxidative stress and tumor potential. Cancer cells do not contain catalase or superoxide dismutase. The theory why vitamin C is so effective against cancer cells is because it produces hydrogen peroxide on the outside and inside of cancer cells, and without superoxide dismutase or catalase, cancer cells can’t defend against it.
It has been shown that hydrogen peroxide and vitamin C have a high affinity for tumor cells, blocking cancer cell metabolism from three pathways, literally starving it to death. Vitamin C attacks the cell membrane, mitochondria and nuclear DNA of a cancer cell by inducing hydrogen peroxide (page 59 Hyperthermia in Oncology). Radiotherapy attacks the cytoplasm and nucleus DNA by increasing hydrogen peroxide. The author stated that “the combination of the two would eliminate any chance for cancer cell survival.”
Vitamin C is selectively targeting tumor cells by increasing hydrogen peroxide around and inside these cells. That is a pro-oxidant effect, like chemotherapy. Chemotherapy increases superoxide and hydrogen peroxide, elucidating the pathway for killing cancer cell. Protecting normal cells against superoxide and hydrogen peroxide should not affect cancer cells and should improve therapy outcome, improve the quality of life during therapy and reduce reoccurrence of cancer.
Grapeseed Extract
To give another example, let’s look at grapeseed extract. Tannic Acid (from grapes) procyanidins (grape seeds) both have been demonstrated to protect against cardiotoxicity from the chemotherapy drugs doxorubicin and anthracycline due to their antioxidant activity. But here is where it gets interesting.
Unlike chemotherapy, grapeseed targets cancer cells while leaving healthy cells alone. While chemotherapy requires large doses to kill advanced stage colon cancer, the opposite is true of grapeseed extract. According to this study, it requires more than half of the grapeseed extract concentration to halt the growth of cancer cells and kill 50% of the stage IV cells than it did to kill the stage II cells. The researchers hypothesized that the grapeseed extract targets colon cancer by introducing oxidative stress, which is programmed cell death. Grapeseed extract is also an inhibitor of the DHFR gene for folate, the same mechanism of the antifolate cancer drug methotrexate.
Niacin
Chemotherapy often causes damage to cells with long-term and short-term regeneration capacities, leading to acute bone marrow suppression and the long-term development of leukemias. Niacin deficiency is common in cancer patients and causes dramatic genomic instability in bone marrow cells in an in vivo rat model. Niacin deficiency delays all of the processes involved in DNA protection and repair which is crucial for cancer prevention. Improvement of niacin status in rats significantly decreased leukemia incidence and suggests that niacin supplementation of cancer patients may decrease the severity of short and long-term side effects of chemotherapy, and could improve tumor cell death.
Niacin is also used in an overmethylated state to bring down high nitric oxide levels. Since most tumors are in a hypermethylated state and nitric oxide plays a role in tumorigenesis, research should explore niacin’s role in tumor hypermethylation.
Grass-Fed Whey Protein
The amino acids in whey protein boost glutathione levels, the body’s major antioxidant system. Glutathione is a doubled edged sword because cancer cells elevate glutathione in their own cells to survive and become drug resistant. However, whey protein lowers cancer cell glutathione levels, allowing the chemotherapy and radiation to be more effective at destroying cancer cells but not to normal cells. Once again, there is a more intelligent process occurring in the body that is beyond the simplistic view of antioxidants.
It would not stand to reason that “antioxidants” are working against chemotherapy because they are protecting healthy cells from hydrogen peroxide and superoxide through superoxide dismutase and catalase activity, an ability a cancer cell does not have. Furthermore, antioxidants and other compounds are targeting cancer cells by introducing oxidative stress selectively to cancer cells, while protecting healthy cells.
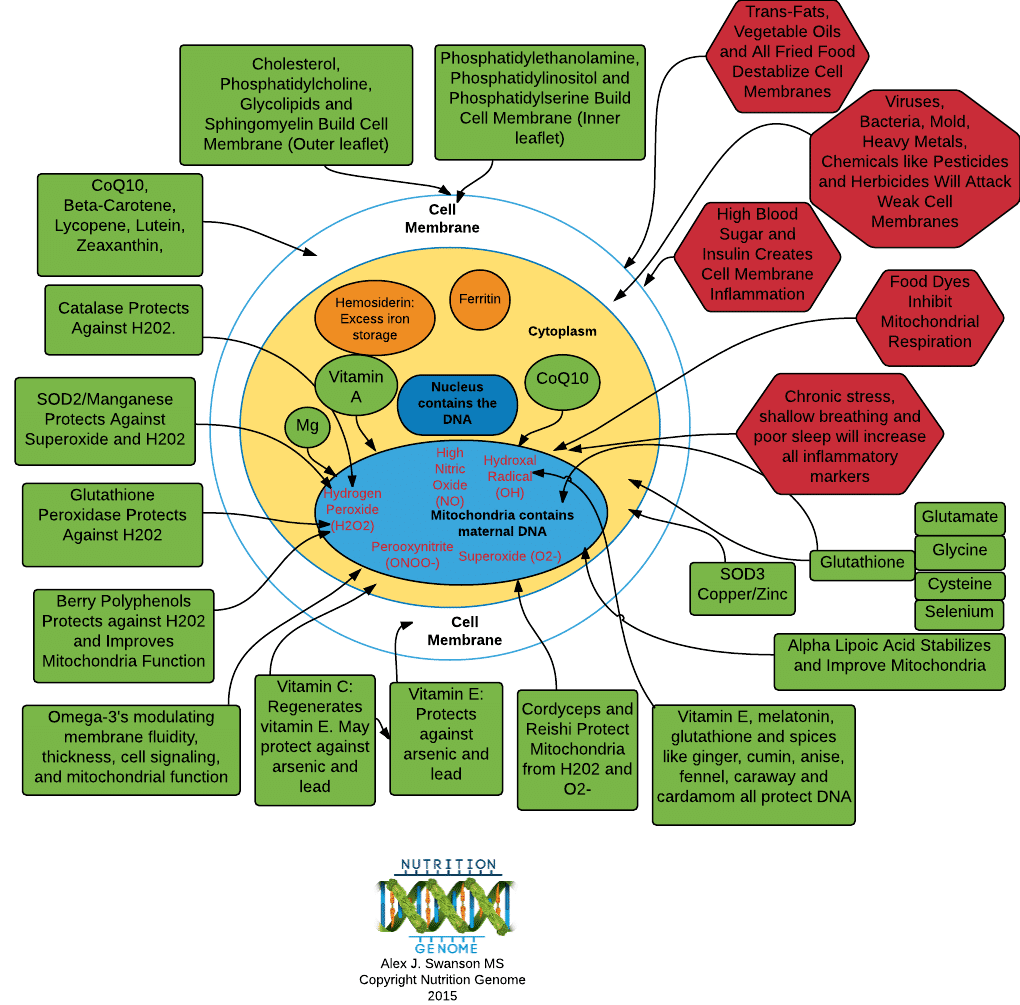
A Visual of the Requirements for a Healthy Cell
Below you can see everything that is required to keep a cell healthy. Now, notice what catalase, glutathione peroxidase and superoxide dismutase are doing. Protecting the mitochondria against hydrogen peroxide right? A cancer cell often fails to do this.

SOD2, SOD3, GSTM1, GSTP1, GPX1, and catalase are all genes that I test through Nutrition Genome and show people which genes need to be strengthened. For example, if you have variants in SOD causing lower activity, you need to be much more conscious of things that lower SOD activity, like fluoridated water.
Significantly lowered levels of reduced glutathione, glutathione peroxidase, superoxide dismutase, and vitamin C and E have all been observed in cancer patients when compared to control subjects. This puts them at a distinct disadvantage for a successful recovery from therapy and the possibility of secondary cancers. In 1997, Dr. Samuel Epstein stated for the Congressional Record that chemotherapy and radiation can increase the risk of secondary cancers by up to 100 times.
Increasing Superoxide Dismutase and Catalase Activity
Increasing superoxide dismutase and catalase activity will help you protect healthy cells from the elevated superoxide and hydrogen peroxide generated by chemotherapy. Superoxide dismutase requires zinc and copper in the right ratios for the cell membrane, while intracellular SOD requires manganese. Cordyceps, reishi, and black cumin seed oil have all been found in studies to protect against and scavenge superoxide. You will also find some of the most impressive anti-cancer research with these three.
Flavonoids, iron (chemotherapy induces anemia), selenium, ginger, cumin, anise, fennel, caraway, and cardamom all assist catalase. Ginger consumption has been reported to decrease lipid peroxidation and normalizes the activities of superoxide dismutase and catalase, as well as GSH and glutathione peroxidase, glutathione reductase, and glutathione-S-transferase. Ginger is also one of the most effective herbs for nausea, common during chemotherapy. All of these have strong antioxidant and anticancer activity.
Fasting and Chemotherapy
From years of research with cancer, I have suspected that one aspect of cancerous growth occurs from overfeeding. This doesn’t necessarily mean obesity, which also increases cancer risk. It means that we do not enter the fasting mode nearly enough to trigger one of the body’s most powerful DNA repair mechanisms that occur when we fast.
Modern studies of fasting how shown tremendous changes that occur after the 13-hour mark, where DNA repair occurs (protecting against cancer). One fascinating study found that fasting protects normal cells, but not cancer cells against high-dose chemotherapy in mice. Fasting prior to chemotherapy often led to more tumor shrinkage than chemo alone, and the combination appeared to eliminate certain kinds of cancer. One study found that women who fasted fewer than 13 hours a night had a 36% higher risk for breast cancer reoccurrence, compared with those who fasted 13 or more hours.
Doing therapy while in the fasting state (aim for 13 hours) and using Gerolsteiner Mineral Water would be the optimal approach if blood sugar issues are not present.
The Best Supplements During Chemotherapy
*Your doctor may or may not approve any of these suggestions, and therefore anything recommended here should be approved by your doctor first. If you only choose one or two items from this list that are not controversial with therapy, it should be the mushrooms.
There is a misconception that medicinal mushrooms interfere with chemotherapy. The exact opposite has been found to be true. As Andrew Weil, MD has stated “They are nontoxic, do not interfere with conventional therapies, and strengthen the body’s defenses.”
Chemotherapy must penetrate the tumor and accumulate within each cell to induce cancer cell death. Medicinal mushrooms have been shown to increase the effects of chemotherapy, usually by increasing the dose of the chemotherapeutic agent that accumulates within a cell. Medicinal mushrooms make chemotherapy work better, reduce the side effects and have a colossal backlog of tumor suppressing and cancer-killing research. The dosage used in research is typically in the 3,00mg to 6,000mg or higher range.
1. Medicinal Mushrooms
Cordyceps
In one study, an orally administered hot-water extract from Cordyceps Sinensis (CS), protected mice from bone marrow and intestinal injuries after total-body irradiation. Even WebMD states, “Cordyceps might improve immunity by stimulating cells and specific chemicals in the immune system. It may also have activity against cancer cells and may shrink tumor size, particularly with lung or skin cancers.”
Cisplatin Chemotherapy Drug: Cordyceps can decrease blood supply to the cancer cell and increase the ability of cisplatin to exert cytotoxic effects. Participants whose combination therapy that included Cordyceps had the longest survival rate.
Reishi
A meta-analysis results showed that patients who had been given reishi (G. lucidum) alongside with chemo/radiotherapy were more likely to respond positively (1.27 times more) compared to chemo/radiotherapy alone, and four studies showed that patients in the G. lucidum group had a relatively improved quality of life in comparison to controls. One study recorded minimal side effects, including nausea and insomnia.
Cisplatin Chemotherapy Drug: Extracts from reishi in the form of ganoderic acid A were recently found to increase accumulation of the chemotherapeutic agent cisplatin inside tumor cells.
Turkey Tail (PSK)
Turkey Tail (PSK) has been shown to provide protection against chemotherapy toxicity. Peripheral neuropathy (ie, nerve damage often occurring in the hands and feet) is a common side effect experienced by colon cancer patients receiving the chemotherapy drugs oxaliplatin, leucovorin, and 5-fluorouracil.
Researchers observed grade 2 or grade 3 peripheral neuropathies in only 4% of colon cancer patients receiving chemotherapy drugs with Turkey Tail (PSK) which is in stark contrast to a 38.4% incidence in those receiving the chemotherapy drugs without PSK. Turkey Tail (PSK) may also have a chemopreventive potential to restrict prostate tumorigenic progression from the hormone-dependent to the hormone-refractory state.
Turkey Tail has been found to protect the immune system’s activity from being suppressed by prolonged use of chemotherapy drugs and the drain from cancer itself. One ten year study of 185 patients with lung cancer showed that combining Turkey Tail with radiation therapy produced satisfactory tumor shrinkage and better survival rates for patients with Stage 1 cancer (39 percent) and Stage II cancer (22 percent) compared to patients with Stage 1 cancer (16 percent) and Stage II cancer (5 percent) who did not take PSK(other studies found in Medicinal Mushrooms: A Clinical Guide.
A meta-analysis of turkey tail by Eliza et al demonstrated an increased rate of survival for cancer patients who took this mushroom, especially participants with breast, gastric, and colorectal cancers.
Docetaxel Chemotherapy Drug: PSK extracted from turkey tail increases the efficacy of the drug docetaxel in the treatment of human gastric carcinoma.
Trastuzumab Chemotherapy Drug: Trastuzumab is a HER2-targeted therapy. When PSK from turkey tail was given with trastuzumab, cell-mediated cytotoxicity was greatly increased. When PSK and trastuzumab were used alone, they had similar rates of tumor inhibition. Combined, these 2 treatments decreased cell growth in tumors by 96%.
Lion’s Mane
One study demonstrated that Lion’s Mane (H. erinaceus) acts as an enhancer to sensitize the chemotherapy drug doxorubicin (Dox) and enhanced intracellular Dox accumulation. The researchers also concluded that induction of natural killer cell activity, activation of macrophages and inhibition of angiogenesis by Lion’s Mane all contribute to the mechanism of reduction of tumor size.
Treatment with a hot water extract of Lion’s Mane decreased lipid peroxidation and increased superoxide dismutase (SOD) and catalase (CAT) activities, quenching free radicals in the gastric tissue of the ethanol-induced rats to exhibit gastroprotective activity.
Maitake
Maitake is thought to exert its effects through its ability to activate various effector cells, such as macrophages, natural killer cells, and T cells, as well as interleukin-1 and superoxide anions.
Research has shown that maitake enhances natural killer cells and prevent cancer progression. One study found that cancer regression or significant symptom improvement was observed in 58.3 percent of liver cancer patients, 68.8 percent of breast cancer patients, and 62.5 percent of lung cancer patients. Furthermore, when maitake was taken in addition to chemotherapy, immune-competent cell activities were enhanced 1.2-1.4 times, compared with chemotherapy alone.
Chaga
Chaga contains a multitude of minerals and is one of the highest sources of superoxide dimutase (SOD) known. In one study, the researchers concluded that Chaga mushroom extracts might represent a valuable source of biologically active compounds with potential for protecting cellular DNA from oxidative damage in human lymphocytes and “affords cellular protection against endogenous DNA damage produced by hydrogen peroxide H2O2.”
Another study concluded that Chaga extract induced the growth inhibition, G0/G1-phase arrest, and apoptosis in human hepatoma HepG2 cells, proving Chaga to be a potential anticancer agent in the treatment of hepatoma. In other studies, long-term administration of Chaga significantly improved the general condition and objective state of patients with uncurable stage III – IV cancer, irrespective of the tumor location.
2. Gerolsteiner Mineral Water
Minerals such as potassium, calcium, sodium, chloride, magnesium, and phosphorus control the balance of fluids within and surrounding cells which is offset by chemotherapy.
On therapy days, prepare according to instructions and sip while undergoing therapy. If using Gerolsteiner and the carbonation bothers you, let it go flat first. It is usually soothing for people. Since water by itself can be nauseating, be sure to add ice and lemon.
3. Grass-Fed Whey
Grass-fed whey concentrate is higher in CLA, a potent anti-cancer compound. Whey protein contains the amino acid precursors glycine, lysine, and glutamine for glutathione (glutamine is needed for repairing the gut which is crucial during chemotherapy), prevents muscle wasting, and provides immunoglobulins for immune system support. This particular product also contains chia seeds (electrolyte rich), MCT oil, probiotics for gut healing, and no sugar or artificial sweeteners.
Use with frozen berries when you get home post-therapy and drink on non-therapy days.
4. Jarrow-Dophilus High Potentcy EPS
Digestion and malabsorption problems are common in patients undergoing chemotherapy since those agents attack all rapidly dividing cells which include the linings of the gastrointestinal tract. Chemotherapy often leads to constipation, and probiotics help prevent constipation.
You may be told by your doctor to avoid lettuce or anything raw that may have bacteria on it. This is because your gut flora is severely compromised, highlighting the importance of balancing gut flora.
5. CoQ10 with Vitamin E
Helps protect the heart during therapy. CoQ10 protects the mitochondria from free radicals and the heart contains the highest concentration of mitochondria. Low blood levels of CoQ10 have been found in patients with myeloma, lymphoma, and cancers of the breast, lung, prostate, pancreas, colon, kidney and head and neck.
Vitamin E has been shown to protect against cardio-myopathies induced by chemotherapy. Vitamin E has also been used in combination with CoQ10 to reduce the side effects of the chemotherapy drug doxorubicin.
6. Seeking Health Niacin Lozenge
See research earlier in the article.
Other Sources
- Hyperthermia in Oncology
- http://www.ncbi.nlm.nih.gov/pubmed/19961266 2. Vitamin C
- http://www.ncbi.nlm.nih.gov/pubmed/12522125 3. Nitric Oxide
- http://www.sciencedirect.com/science/article/pii/S2213231712000067 4. NOS1,2,3:
- http://www.diabetesincontrol.com/wp-content/uploads/2015/10/nitric-oxide.pdf?5. Flavonoids:
- http://www.sciencedirect.com/science/article/pii/S000527280900190X 6. Oxidized LDL:
- http://www.ncbi.nlm.nih.gov/pubmed/8653881 7. Pomegranates: Aviram M, Rosenblat M, Gaitini D, et al. Pomegranate juice consumption for 3 years by patients with carotid artery stenosis reduces common carotid intima-media thickness, blood pressure and LDL oxidation. Clin Nutr. 2004 Jun;23(3):423-33. 8. Mg:
- http://www.ncbi.nlm.nih.gov/pubmed/26114348
- Vitamin C and OH: http://www.ncbi.nlm.nih.gov/pubmed/26237409
- Black Cumin Seed: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2583426/
- Rosemarinic Acid http://www.ncbi.nlm.nih.gov/pubmed/17420060







Recent Comments